Learn how to know if you have Candida overgrowth, and get the latest recommendations about diet and natural treatment for yeast overgrowth!
Note from Dena: I’m excited to share this guest post on such an important topic. It was written by Marla Ramos, Dietetic Intern, as part of a research partnership between Back To The Book Nutrition and post-graduate nutrition students from the University of Houston.
Our gut health is crucial to our overall health.
A healthy gut is teeming with a variety of bacteria, yeasts, and other organisms living in harmony with one another. But, when Candida or other normal gut “residents” are allowed to overgrow, it can lead to nagging symptoms and chronic health conditions.
WHAT IS CANDIDA OVERGROWTH?
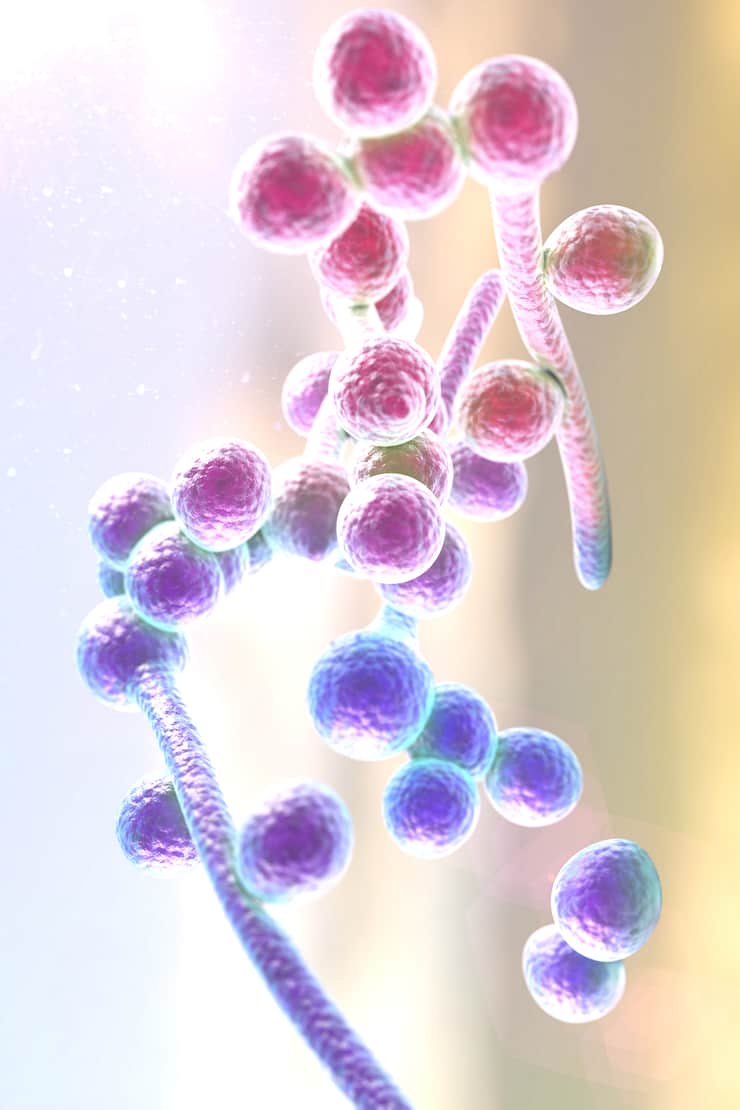
Candida overgrowth, also known as Candidiasis or Candida Overgrowth Syndrome, is as the name states, an overgrowth of yeast, typically Candida albicans (aka Candida). (1) Candida albicans is the most common disease-causing species of Candida, although there are other forms of Candida and even other forms of yeast (i.e., Geotrichum) that can overgrow.
WHAT CAUSES CANDIDA OVERGROWTH?
Candida albicans is a normally harmless yeast found in mucus membranes, including those in the mouth, ears, nose, skin, vagina, and gut. Overgrowth can occur in any of these areas, often in combination with one another, so identification of any one area of overgrowth may indicate the presence of overgrowth in the gut as well.
MEDICATION AND LIFESTYLE FACTORS THAT CONTRIBUTE TO A CANDIDA OVERGROWTH (1, 2, 17, 18)
No one factor on this list causes Candida overgrowth on its own. But, in combination, these factors can create the perfect storm for an overgrowth.
- Diet high in refined carbohydrates (white flour/white rice), and sugar
- Diet high in certain fermented foods like Kombucha, sauerkraut, and pickles
- High alcohol intake
- High or chronic stress environment (prolonged stress can suppress immune function and promote digestive imbalance)
- Suppressed immune system
- Low stomach acid (strong acid production helps prevent yeast overgrowth in the upper digestive tract)
- Poor bile flow (bile is antimicrobial)
- Overuse of antibiotics (number 1 reason, particularly broad-spectrum antibiotics like tetracycline, cephalexin, cefoperazone)
- Oral contraceptives (birth control pill)
- Oral corticosteroid use (Prednisone, etc.)
- Inhaled steroids (steroid asthma inhaler, steroid nasal sprays)
- Inflammatory conditions (obesity, autoimmune disease, etc.)
- Pregnancy
- Diabetes
- Mold exposure
CONDITIONS ASSOCIATED WITH CANDIDA (2, 4, 7)
- ADD/ADHD
- Eczema
- Psoriasis
- Hives
- Rash
- Hashimoto’s Thyroiditis
- Rheumatoid Arthritis
- Ulcerative Colitis (70-86%)
- Crohn’s Disease (44%)
- Lupus
- Scleroderma
- Multiple Sclerosis
- Fibromyalgia
- Chronic Fatigue Syndrome
- IBS
- Depression/Anxiety
- Leaky Gut Syndrome
- Chronic Inflammation
- Asthma
- Obesity
- Diabetes
HOW DO I KNOW IF I HAVE CANDIDA?
Candida overgrowth can manifest in a variety of symptoms, some of which can be non-specific and similar to other conditions – making it difficult to diagnose based on symptoms alone.
COMMON SYMPTOMS OF CANDIDA
- Recurrent athlete’s foot
- Recurrent toenail fungus
- Recurrent yeast infections (Vaginal Candidiasis)
- White coating on tongue (Oral Thrush)
- Feeling tired and worn down
- Gas/Bloating
- Diarrhea/Constipation
- Brain fog
- Headaches or migraines
- Skin rashes or other skin issues (16)
- Irritability/Mood swings
- Depression/Anxiety
- Diagnosed autoimmune diseases
- Recurring UTIs
- Rectal itching
- Vaginal itching
- Dandruff
- Severe seasonal allergies
- Itchy ears
- Sugar cravings
- New sensitivities to commonly eaten foods (16)
- Disorientation
- Dizziness
- Muscle and joint aches
- Chronic sinusitis
- Recurrent colds
- PMS
- Decreased libido
- Prostate and bladder infections
HOW TO TEST FOR CANDIDA
It’s important to confirm a Candida infection, and not just treat based on symptoms, the latter of which can lead to costly and unnecessary medication use and unwarranted diet restrictions.
It is best to use at least one of the following tests, along with your symptoms, to confirm a diagnosis of Candida or other yeast overgrowth. A holistic dietitian or other qualified healthcare provider can help determine whether Candida is causing symptoms, and can order any or all of the following tests.
- Blood Test – Checks for high levels of IgG, IgA, and IgM (Candida antibodies).
- Stool Test – Checks for actual yeast in the stool. Positive test is indicative of Candida in your colon, or large intestine. My (Dena’s) preferred stool test is the GI MAP test from Diagnostic Solutions. All Holistic Nutrition Clients have access to this comprehensive, at home test.
- Urine Test – Checks for D-arabinitol (a yeast waste product). A positive test is indicative of Candida in the small intestine.
Note from Dena:
If you don’t already have a practitioner who can order these tests and discuss the results with you, I’d love to help! Schedule a free, 10 minute Discovery Call to get started!
There is also a fourth test, a spit test (2), which can be performed at home and the best part is, it’s free. This test could be a good starting point if you suspect you might have a Candida overgrowth, but the spit test shouldn’t be used to diagnose Candida.
To perform the spit test – First thing in the morning (before eating, drinking, or brushing your teeth), spit into a clear glass of water. If after 15-30 minutes your spit looks cloudy, has grown legs, or sinks to the bottom, then you might have Candida. Doing this over the course of a few days might paint a better picture. This video shows how to perform the spit test. Again, it’s important to confirm with one of the more established and scientific tests mentioned above before treating.
Note: This post contains affiliate links. By making purchases through these links, you pay the same amount for products, but a small portion of the sale will be sent my way to help support the mission of Back To The Book Nutrition. Thank you!
HOW TO TREAT CANDIDA?
It’s important to reiterate that the goal is not to eliminate Candida entirely, but to reduce overgrowth.
There are several approaches to stopping the yeast overgrowth that include diet, natural antimicrobials, and prescription antifungals. A combination of these seems to be most effective.
The “Candida Diet”
I don’t believe extreme restriction as advocated by some “anti-Candida diets” is necessary, but cutting back in certain areas can help get the overgrowth under control initially.
- Cut down on sugar – Yeast thrives on sugar! Eliminate candy, sweets, alcohol, refined flours, and sweetened beverages, and consider temporarily removing fruits, honey, and other natural sugars as well.
- Moderate complex carbs – Complex carbohydrates like whole grains, beans, lentils, and potatoes are healthy, but make sure you’re not overdoing them since excess carbohydrate intake can fuel yeast overgrowth and should be limited during Step 1.
- Limit fermented foods? – There is limited data in this area and experts differ in their opinions about whether fermented foods should be consumed. I’ve had multiple clients feel that kombucha in particular triggers Candida symptoms.
- Consider avoiding certain nuts/nut butters? – I generally don’t recommend this, but some practitioners suggest omitting peanuts, cashews, pecans, walnuts, and pistachios tend to be highest in mold/fungus
- Consider avoiding certain forms of dairy – Again, I don’t usually recommend this, but some practitioners advocate for avoidance of dairy due to its natural sugar content, but scientific data to support this claim is limited. (2)
As always, discuss personal recommendations with a holistic dietitian or other licensed provider.
Medical Treatment to Help Stop Candida Overgrowth
Both prescription medications and natural antimicrobials and antifungals can be used to treat Candida.
- Prescription Medications
- Nystatin (preferred for intestinal yeast)
- Diflucan (more common for yeast overgrowth outside the intestines – vaginal, etc.)
There are several antifungal medications available. While successful in treating Candida overgrowth infections, one study has shown resistance of Candida albicans to antifungal medication, and this is a growing concern among practitioners as use of these medications becomes more widespread. (9)
Natural Antimicrobials and Antifungals
- Caprylic acid (found in coconut oil and in the probiotic S. boulardii) (11, 12, 16)
- Undecylenic acid (10)
- Lavender oil (13)
- Garlic oil (19)
- Oregano oil (20)
- Grapefruit seed extract (GSE) (21)
These are just a few of the most well supported botanicals and essential oils that can be used in the fight against Candida, and most practitioners elect to use a combination of them for best results.(2,5) It’s important to remember that some of these may have side effects or interactions with other medications or conditions. Most will also have antibacterial effects, which could be helpful in some cases but harmful in others. Always consult with your licensed practitioner for personal recommendations.
Die-off and other Cautions About Medical Treatment for Candida Overgrowth
Die-off reactions can occur as a result of medical treatment for Candida and other yeasts. As yeasts die off and toxic byproducts are released, you may experience temporary symptoms that include nausea, fatigue, or flu-like symptoms. Starting at lower doses (if using herbal products) and increasing toward the recommended dose gradually can help minimize or avoid die off altogether.
Mild die-off symptoms are usually harmless and should pass within a few days. (1, 27) Be sure to drink plenty of water to help your body rid itself of the dead yeast and toxins, and consult your provider if symptoms linger.
HOW CAN I PREVENT CANDIDA RECURRENCE?
Once Candida overgrowth is effectively treated, it’s important to make adjustments to prevent yeast overgrowth from recurring.
- Avoid unnecessary antibiotics (antibiotics only treat bacterial infections, not the common cold or the flu, which are caused by viruses)
- If you must take antibiotics, take a probiotic supplement 2-3 hours after each dose, and for several months after you finish your antibiotics.
- Limit oral contraceptive use
- Limit nasal steroid use, and rinse your mouth after each use of your steroid inhaler
- Manage blood sugar and consider getting checked for diabetes
- Reduce and manage stress
- Exercise regularly to strengthen your immune system, but don’t overdo it
- Eat a nutrient-dense, whole food diet
- Increase your dietary fiber (feeds healthy yeast and bacteria, stimulates regular bowel movements, and helps your body eliminate the yeast and its toxins)
- Consume probiotic-rich foods, including plain yogurt or kefir with live active cultures, and lacto-fermented vegetables
- Consider taking a high quality probiotic supplement (1)
Check out these other great posts on gut health!
20 Natural Remedies for Heartburn, Reflux, & GERD
The Best Diet for SIBO…and why diet alone won’t fix it
About the author: Marla Ramos is a Dietetic Intern, with a B.S. in Human Nutrition and Foods from the University of Houston. She has a particular interest in gut health due to her own personal experience with Crohn’s Disease.
Disclaimer: Information on this site is intended only for informational purposes and is not a substitute for medical advice. Always consult with a trusted healthcare provider before implementing significant dietary change. Read additional disclaimer info here.
References
- Candida Overgrowth Syndrome. WholeHealth Chicago, Integrative, Functional, and Alternative Medicine.
- Myers, A. (2013) 10 Signs you have candida overgrowth & what to do about it.
- Chronic intestinal candidiasis as a possible etiological factor in the chronic fatigue syndrome (1995). Med Hypotheses. 55:6, 507-515.
- Zwolinska-Wchislo, M., et al. (2006). The influence of Candida albicans on the course of ulcerative colitis. Przegl Lek, 63:7, 533-8.
- Kresser, Chris (2015). Top 4 mistakes people make when treating candida overgrowth.
- Myers, A. (2012) How to heal your gut and heal yourself. Mindbodygreen.
- Kumamoto, C. (2011) Inflammation and gastrointestinal Candida colonization. Current Opinion in Microbiology, 14:4, 386-391.
- Hamad, M, et al. (2006). Utility of the oestrogen-dependent vaginal candidosis murine model in evaluating the efficacy of various therapies against vaginal Candida albicans infection, Mycoses, 49, 104-108.
- Mobile, C., and Johnson, A. (2015) Candida albicans biofilms and human disease. Annual Review of Microbiology, 69, 71-92.
- Shi, D., et al. (2016) Antifungal effects of undecylenic acid on the biofilm formation of Candida albicans, International Journal of Clinical Pharmacoloy and Therapeutics, 54: 5, 343-353.
- Ogbolu, D., et al. (2007) In vitro antimicrobial properties of coconut oil on Candida species in Ibadan, Nigeria, Journal of Medicinal Foods, 10:2, 384-387.
- Murzyn, A., et al. (2010) Capric acid secreted by S. boulardii inhibits C. albicans filamentous growth, adhesion and biofilm formation.
- D’Auria, F., et al. (2005) Antifungal activity of Lavandula angustifolia essential oil against Candida albicans yeast and mycelial form, Medical Mycology, 43:5, 391-396.
- Ducluzeau, R., Bensaada, M., Comparative effect of a single or continuous administration of Saccharomyces boulardii on the establishment of various strains of candida in the digestive tract of gnotiotic mice, Annals of Microbiology, 133:3, 491-501.
- Yamaguchi, N., et al. (2006), Gastrointestinal Candida colonization promotes sensitization against food antigens by affecting the mucosa barrier in mice, Gut, 55:7, 954-960.
- Matsubara, V., et al. (2016) Probiotic lactobacilli inhibit early stages of Candida albicans biofilm development by reducing the growth, cell adhesion, and filamentation, Applied Microbiology and Biotechnology, 100:14, 6415-6426.
- Takahashi, M., et al. (2012) Inhibition of Candida mycelia growth by a medium chain fatty acids, capric acid in vitro and its therapeurtic efficacy in murine oral candidias, Medical Mycology Journal, 53:4, 255-61.
- Tarry, W., Fisher, M., Shen, S., Mawhinney, M. (2005), Candida albicans: the estrogen target for vaginal colonization, The Journal of Surgical Research, 129:2, 278-282.
- Erb, J., et al., (2013) Modulation of post-antibiotic bacterial community reassembly and host response by Candida albicans, Scientific Reports, 3:2191, doi: 10.1038/srep0291.
- Li, W. Shi, Q., et al. (2016) Antifungal activity, kinetics and molecular mechanism of action of garlic oil against Candida albicans, Science Reports, 6:22805. Doi: 10.1038/srep22805.
- Bona, E., et al. (2016) Sensitivity of Candida albicans to essential oils: are they an alternative to antifungal agents, Applied Microbiology, 121:6, 1530-1545.
- Han, Y. (2007), Synergic effect of grape seed extract with amphotericin B against disseminated candidiasis due to Candida albicans, Phytomedicine: International Journal of Phytotherapy & Phtyopharmacology, 14:11, 733.
- Cummings, J., Macfarlane, G. (2002), Gastrointestinal effects of prebiotics, The British Journal of Nutrition, 87:2, A145-151.
- Slavin, J, Fiber and prebiotics: mechanisms and health benefits, Nutrients, 5:4, 1417-1435 doi: 10.3390/nu5041417.
- Dr. Axe, 7 Reasons to get prebiotics in your diet – plus best sources.
- Singh, A., Verma, R., Murari, A., Agrawal, A., (2014), Oral candidiasis: an overview, Journal of Oral Maxillofacial Pathology, 18:1, S81-S85.
- Spnucci, G., et al. (2006) Endogenous ethanol production in a patient with chronic intestinal pseudo-obstruction and small intestinal bacterial overgrowth, European Journal of Gastroenterology & Hepatology, 18:7, 799-802.
- Gainza-Cirauqui, M., et al., (2013) 42:3, 243-249, doi: 10.1111/j.1600-0714.2012.01203x.

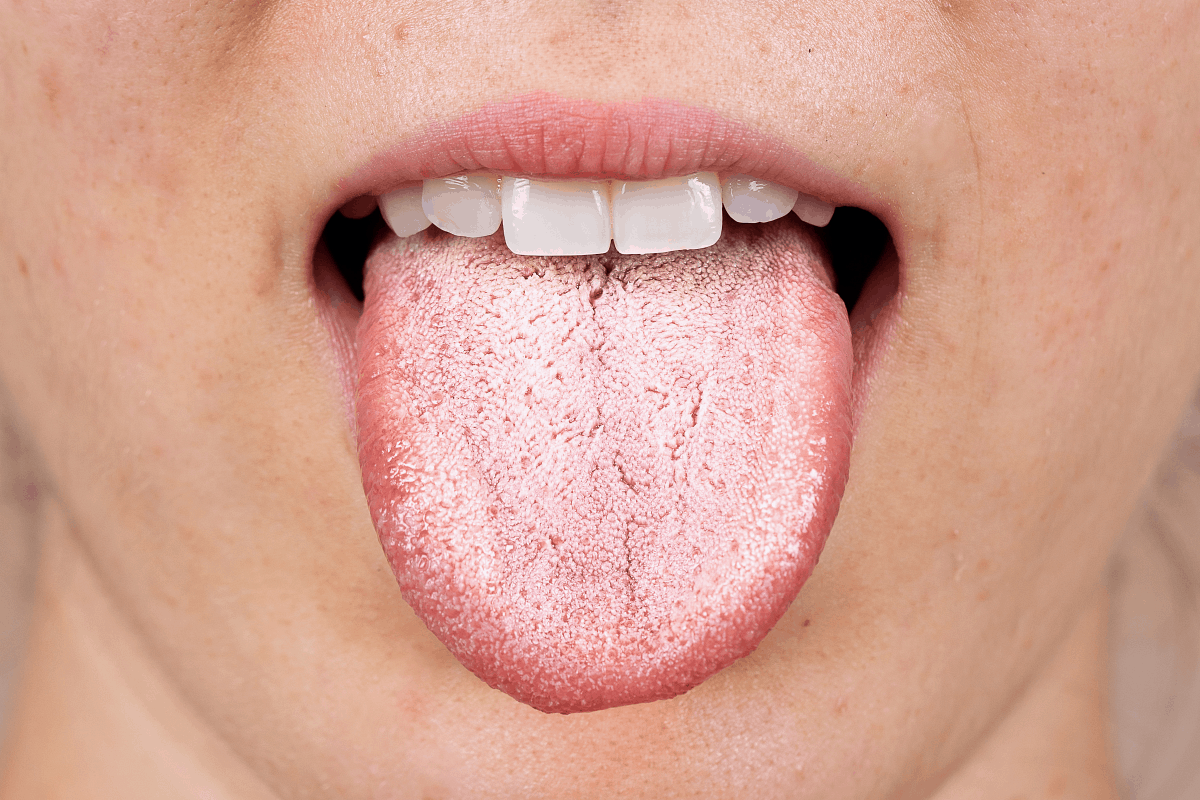






very informative article. Thank you.
I don’t know much about this condition but it’s a good thing that there’s a way to handle this.
I’ve been wondering for a while if I have a candida overgrowth. I have many symptoms.
Rachel, we would like to help! You can jump on a free 10min call with us here:FREE CALL
There was a time that this was a struggle for me because I was pregnant and nursing at the same time. My poor body couldn’t balance it all! And once the balance is off, it’s hard to get it back together again! Fortunately once I did, the problems disappeared and haven’t been back!
This is a great post for those who are struggling with yeast issues.
Thanks for sharing with us Marie!
m not aware of this kind of infection. Thanks for sharing the knowledge.
Treating something naturally and properly is always a plus for me!
Very informative post. Prevention is key in treating any chronic condition. Thanks for sharing
Most of this information is new to me but SO helpful, thanks!
great information you have mentioned here…glad you shared such valuable and useful blog post with us..great work though…found it so informative…
I’ve never heard of candida before. Nice to know there’s a natural treatment for it.