Learn the best diet for Graves’ Disease, including specific foods to reduce inflammation and autoimmunity, support the thyroid, and promote gut health. Plus, a list of research backed natural supplements for hyperthyroidism.

Note from Dena: This post was co-written by Khadija Hamid, Dietetic Intern, as part of a research partnership between Back To The Book Nutrition and post-graduate nutrition students from the University of Houston.
Graves’ disease – or autoimmune hyperthyroidism – is the most common cause of overactive thyroid in the United States, accounting for 60%-80% of all cases. It most frequently strikes between the ages of 20 and 50 but can occur at any age, and is 7-8 times more common in women than in men.
In Graves’ Disease, similar to in Hashimoto’s Thyroiditis (autoimmune hypothyroidism), the immune system attacks the thyroid; but, unlike Hashimoto’s, Graves’ causes the thyroid to produce more thyroid hormone than the body needs, not less. (1)
SYMPTOMS OF GRAVES’ DISEASE & HYPERTHYROIDISM
Individuals with Graves’ Disease often have symptoms similar to non-autoimmune hyperthyroidism, such as:
- Faster heart rate
- Frequent bowel movements or diarrhea
- Feeling hot all the time
- Nervousness or irritability
- Increased appetite
- Unintentional weight loss
- Fatigue
- Muscle weakness
- Hand tremors
- Insomnia
- Hair loss
- Changes in menstrual cycles
Clues that Hyperthyroidism is Caused by Graves’ Disease
Having one or more of these symptoms makes it more likely that Graves’ Disease is driving hyperthyroidism.
- Goiter – A swelling in the lower front portion of the neck caused by an enlarged thyroid gland. (3) Goiter can cause difficulty swallowing, a hoarse voice, or a visible lump in the neck, but can be present even if none of these occur.
- Graves’ Eye Disease – Graves’ disease can cause swelling of tissues around the eyes in approximately 50% of patients. The eyes bulge out and eyelids appear to be pulled back. The person may have double vision, itching, and/or weeping of the eyes (2).
- Swollen, Dark, or Itchy Skin – “Graves’ Dermopathy” is a swelling or reddening of the feet and shins. The skin may appear thicker and darker than normal skin, and it may itch. (3)
- Thyroid Storm – In cases of severe hyperthyroidism, such as can occur with Graves’ Disease, this rare but life threatening episode with intense heart pounding and increases in blood pressure and body temperature. If you experience these symtoms, seek medical attention immediately.
- History of Mononucleosis or Epstein Barr Virus (EBV) – Those who’ve had these appear to be more likely to develop Graves’ Disease. (12)
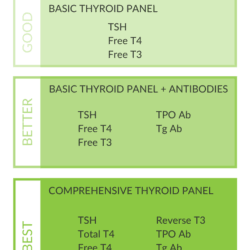
Common Laboratory Tests in Graves’ Disease
In addition to symptoms, the following are common lab results in Graves’ Disease. It’s still possible to have Graves’ Disease even if all of these are not present.
- Very Low Thyroid Stimulating Hormone (TSH) (Blood test) – If you have Graves’ disease, your TSH level will probably be <0.5 because the pituitary gland will reduce its production of TSH in an attempt to get the thyroid to produce less thyroid hormone. (4)
- High Thyroid-stimulating Immunoglobulin (TSI) (Blood test) – TSI is an antibody (immunoglobulin) in the blood that can bind to TSH receptors and raise thyroid hormone (T4 and T3) levels. TSI is present in 90% of Graves’ disease patients. (9)
- High Thyroid Peroxidase (TPO) Antibodies (Blood test) – Thyroid Peroxidase (TPO) enzyme plays an important role in the production of the thyroid hormones. High TPO antibodies suggests that the cause of thyroid disease is an immune disorder, such as Hashimoto’s disease or Graves’ disease. 80% of Graves’ disease patients have high TPO levels. (9)
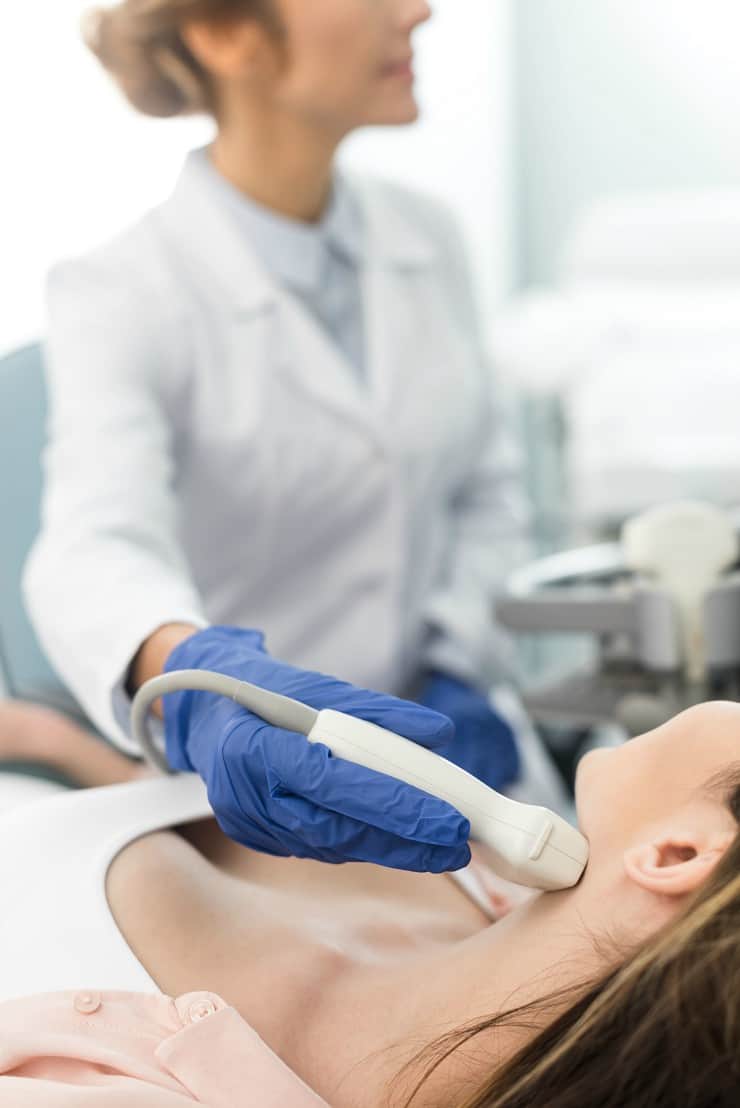
- Thyroid Nodules on Ultrasound (In office imaging) – Nodules are common in Graves’ Disease. If nodules are found, it’s common to biopsy them to rule out thyroid cancer.
- High Radioactive Iodine Uptake (RAIU) test (In-office scan) – A pill or liquid containing radioactive iodine is given, then a scanner measures the amount of iodine the thyroid absorbs from the bloodstream and determines if all or only part of the thyroid is overactive. (4)
THE PROBLEM WITH CONVENTIONAL GRAVES DISEASE TREATMENT
In the conventional medical model, Graves’ Disease is treated with medications or therapies to suppress thyroid function. In many cases, the thyroid is removed altogether.
These efforts will only silence the symptoms of autoimmune thyroid disease, but the underlying autoimmunity is still present. Sadly, it’s common for individuals who do not address their autoimmunity to later develop additional autoimmune conditions like Rheumatoid Arthritis, Lupus, and others.
A more effective approach to Graves’ Disease and other autoimmune conditions is to consider the target organ (the thyroid gland, in the case of Graves’ Disease) the victim, not the criminal. The autoimmunity itself is the criminal and it will continue finding other victims until it is stopped.
This doesn’t mean prescription medications or medical treatment is never needed, but the approach should emphasize addressing the root causes and minimize the need for harsh medications and invasive therapies.
THE BEST GRAVES’ DISEASE DIET
Fortunately, autoimmunity is very responsive to diet, supplements, and lifestyle measures. The best diet for Graves’ Disease is one that supports proper thyroid function and addresses the autoimmunity – one that:
- Reduces inflammation
- Optimizes gut health
- Supports proper immune function
- Is nutrient dense, including nutrients that support the thyroid
- Is gluten free since the gluten molecule is similar enough to thyroid tissue that the immune system can get confused and attack the thyroid in respose to gluten exposure (this is called “molecular mimicry”)
- Includes very few processed foods
The Autoimmune Protocol (AIP) for Graves’ Disease
AIP meets all the criteria above and has been shown to induce remission of various autoimmune conditions, making it a great consideration for Graves’ Disease. AIP is a gluten free, grain free, dairy free diet that emphasizes nutrient dense whole foods and minimizes foods that trigger autoimmunity (eggs, nightshades, nuts. etc.).
Ideally, one would do the elimination and reintroduction version of AIP to help identify their personal triggers be able to re-incorporate as many different foods as possible.
Learn more about AIP and get links to my favorite AIP resources here!
Can Goitrogenic Foods Improve Graves’?
Goitrogens are natural compounds in certain foods that interfere with thyroid hormones. Theoretically, eating a few servings of these daily – especially in raw form – could help reduce thyroid hormone production. But, using goitrogens therapeutically hasn’t been well proven in scientific studies and shouldn’t be considered a stand-alone treatment for Graves’ Disease.
Foods high in goitrogens include:
- Cruciferous vegetables (broccoli, cauliflower, kale, Brussels sprouts, cabbage, arugula, etc.)
- Seaweed/kelp
- Cassava
- Sweet potato
Are high iodine foods bad for Graves’ Disease?
The role of iodine is controversial since both too little and too much iodine intake can cause goiter and other thyroid problems. Eating large quantities of iodine rich foods daily (seaweed/kelp, fish and seafood, dairy, processed foods with lots of iodized salt added, etc.) may make Graves’ worse since it could cause thyroid glands to produce more thyroid hormones.
GRAVES’ DISEASE SUPPLEMENTS TO CONSIDER
Speak to your practitioner before trying supplements, particularly if you have other health conditions.
- High quality daily multivitamin– This should include vitamins A, C, D, E, K-2 and methylated B vitamins, as well as trace minerals like magnesium, calcium, iron, zinc, and selenium (10).
- Vitamin D – Graves’ Disease patients are much more likely to be deficient in vitamin D and additional vitamin D (preferably in combination with vitamin K-2) can help optimize vitamin D levels. 2,000-5,000 IU/day is common for correcting low vitamin D levels.
- Omega-3’s – High-quality fish oil supplements are the best source of omega-3’s to help reduce inflammation (8). 1,000-4,000 mg/day is a common dose.
- L-Carnitine – May help with the symptoms of hyperthyroidism, including heart palpitation, tremors, and fatigue (7). 500 mg/day is a common dose.
- Selenium – Selenium has been shown to improve symptoms of Graves’ Disease and thyroid storm, and may even improve response to medications used for Graves’ (13). My Daily Foundation multivitamin-mineral includes 200 mcg selenium but, if the mutlivitamin you take doesn’t, be sure to add selenium to your supplement regimen. 200 mcg is a common dose.
- High potency Probiotics– to help optimize gut health and immune function (1). 25-100 billion CFU/day is a common dose.
- Bugleweed – Bugleweed inhibits TSH so less thyroid hormone is produced, and it can decrease TSH antibodies. It is helpful for symptoms such as palpitations, convulsions, tremors, anxiety, and insomnia (6). Doses vary.
- Lemon Balm – Lemon balm helps to normalize the overactive thyroid. It reduces the levels of stress hormone and promotes relaxation and counter feelings of tension and anxiety (5). Doses vary.
- Motherwort – In autoimmune disease, it reduces the inflammation and can be used to address the heart conditions including, heart failure, irregular heartbeat, and anxiety (7). Doses vary.
Supplements to avoid with Graves’ Disease
- Iodine – Iodine supplementation in thyroid disease is contraversial. Most holistic practitioners discourage iodine supplements in Graves’ Disease since excess iodine can make hyperthyroidism worse. Talk with your practitioner about whether or not to take iodine supplements.
STRESS, GUT HEALTH, AND IMMUNE FUNCTION
Diet and supplements are key for living well with the autoimmune disease but, for the best results, you also need to address underlying root causes that gave rise to autoimmunity in the first place, such as chronic stress, poor gut health, and immune dysfunction.
Consider working with a practitioner experienced in autoimmune conditions to help you test for and overcome imbalances in your HPA stress axis, bacterial overgrowth in the gut, repair a leaky gut, resolve food sensitivities, replete nutrient insufficiencies, and other individual factors that may be triggering autoimmune activity in your body.
Check out these other great articles!
Which Thyroid Tests You Need + Where to Get Them
8 Best Nutrients + Foods for Thyroid Health
Best Autoimmune Diet + Lifestyle Tips
About the Co-Author
Khadija Hamid is a Dietetic Intern at the University of Houston. She graduated from Masters in Healthcare Leadership and Management from University of Texas at Dallas. Her goal is to use nutrition and food science to make a positive impact by improving community’s health.
Disclaimer: Information on this site is intended only for informational purposes and is not a substitute for medical advice. Always consult with a trusted healthcare provider before implementing significant dietary change. Read additional disclaimer info here.
References
- Wiersinga W. M. (2019). Graves’ Disease: Can It Be Cured?. Endocrinology and metabolism (Seoul, Korea), 34(1), 29–38. https://doi.org/10.3803/EnM.2019.34.1.29
- McAlinden C. (2014). An overview of thyroid eye disease. Eye and vision (London, England), 1, 9. https://doi.org/10.1186/s40662-014-0009-8
- Safer J. D. (2011). Thyroid hormone action on skin. Dermato-endocrinology, 3(3), 211–215. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3219173/
- De Leo, S., Lee, S. Y., & Braverman, L. E. (2016). Hyperthyroidism. Lancet (London, England), 388(10047), 906–918. https://doi.org/10.1016/S0140-6736(16)00278-6
- Lai, J., Hunter-Orange, J., & Clemens, K. K. (2019). Hyperthyroidism following the ingestion of natural health products. Canadian family physician Medecin de famille canadien, 65(9), 634–635. https://europepmc.org/article/med/31515312
- Yarnell, Eric & Kathy. (2006). Botanical Medicine for Thyroid Regulation. Alternative and Complementary Therapies. 12. 107-112. 10.1089/act.2006. 12. 107. https://www.researchgate.net/publication/244889874_Botanical_Medicine_for_Thyroid_Regulation
- Fierascu, R. C., Fierascu, I., Ortan, A., Fierascu, I. C., Anuta, V., Velescu, B. S., … Dinu-Pirvu, C. E. (2019). Leonurus cardiaca L. as a Source of Bioactive Compounds: An Update of the European Medicines Agency Assessment Report (2010). BioMed Research International, 2019, 1–13. https://www.hindawi.com/journals/bmri/2019/4303215/
- NIH Fact Sheet: Omega 3 Fatty Acids. https://ods.od.nih.gov/factsheets/Omega3FattyAcids-HealthProfessional
- Fröhlich, E., & Wahl, R. (2017). Thyroid Autoimmunity: Role of Anti-thyroid Antibodies in Thyroid and Extra-Thyroidal Diseases. Frontiers in immunology, 8, 521. https://doi.org/10.3389/fimmu.2017.00521
- Sworczak K, Wiśniewski P. The role of vitamins in the prevention and treatment of thyroid disorders. Endokrynol Pol. 2011;62(4):340–344. https://www.ncbi.nlm.nih.gov/pubmed/21879475
- Xu, M. Y., Cao, B., Yin, J., Wang, D. F., Chen, K. L., & Lu, Q. B. (2015). Vitamin D and Graves’ disease: a meta-analysis update. Nutrients, 7(5), 3813–3827. https://doi.org/10.3390/nu7053813
- Pyzik, A., Grywalska, E., Matyjaszek-Matuszek, B., Ludian, J., Kiszczak-Bochyńska, E., Smoleń, A., Roliński, J., & Pyzik, D. (2019). Does the Epstein-Barr Virus Play a Role in the Pathogenesis of Graves’ Disease?. International journal of molecular sciences, 20(13), 3145. https://doi.org/10.3390/ijms20133145
- Xu, B., Wu, D., Ying, H., & Zhang, Y. (2019). A pilot study on the beneficial effects of additional selenium supplementation to methimazole for treating patients with Graves’ disease. Turkish journal of medical sciences, 49(3), 715–722. https://doi.org/10.3906/sag-1808-67






Thanks for sharing. I am one of the rare younger men diagnosed with Graves Hyperthyroidism. Was hospitalized with a heartrate of 170 in atrial fibrillation before finally getting a diagnosis. Despite being an athlete in excellent health, Graves took hold. The disease is difficult to say the least and can negatively impact almost every area of your life. Anxiety and stress become nearly unmanageable at times. Physical symptoms are awful; However, modern endocrinology has very limited approaches to this. It is very helpful to find information on things we can do in addition to the limited treatments available. Thank you… Read more »
I’m so glad the article was helpful, Chris. Thank you for sharing your story – I agree, Graves’ is underrepresented in the thyroid discussion, and we need to get the word out about a more holistic and thorough approach to managing it.
I will be sharing this to my uncle who has graves disease! This was very helpful and insightful.
I have never really heard of Graves Disease before. Thank you for bringing awareness to the disease and bring relief for those who need it!
This was a very informative post and I am sure that people who suffer from this disease will find it very helpful. Diet has a direct connection to our health.
Thanks for the comment Joanna!
By eating healthy food we can be safe from nowadays diseases……. it is very informative blog.
Thanks for the comment!
I’am working my diet but after reading this article I’ve learn a lot about the graves disease thanks to this!
Glad you found it informative!
To be honest, this is the first time I heard of Graves Disease. Thanks for shedding light on this 🙂
Happy to hear that you found it to be informative!
I’ve never really heard of graves disease. Thanks for the info. I also like treating myself naturally, usually with diet.
Good to hear Jon, and thank you for commenting!
Thanks for creative awareness about this disease. This is very informative post and I am sharing in some of my FB groups
Thank you so much for sharing!
I am thankful for sharing this article about hypothyroidism. Sometimes, metabolic disease is not easily recognizable because the physical manifestation is not apparent.
Glad you like it Ramil!