Everything you need to know about Leaky Gut – what causes it, how to know if you have it, and how to fix it naturally!
Note from Dena: This post was co-written with Lauren McNamara, Dietetic Intern, as part of a research partnership between Back To The Book Nutrition and post-graduate nutrition students from the University of Houston.
Seemingly unrelated symptoms – constant bloating, acne that reminds you of your teenage years, brain fog, joint pain, chronic fatigue – could actually have a common thread. This mixed bag of symptoms is somewhat of a plague these days, and might all be resulting from leaky gut.
What is Leaky Gut?
In short, leaky gut is an increased intestinal permeability.
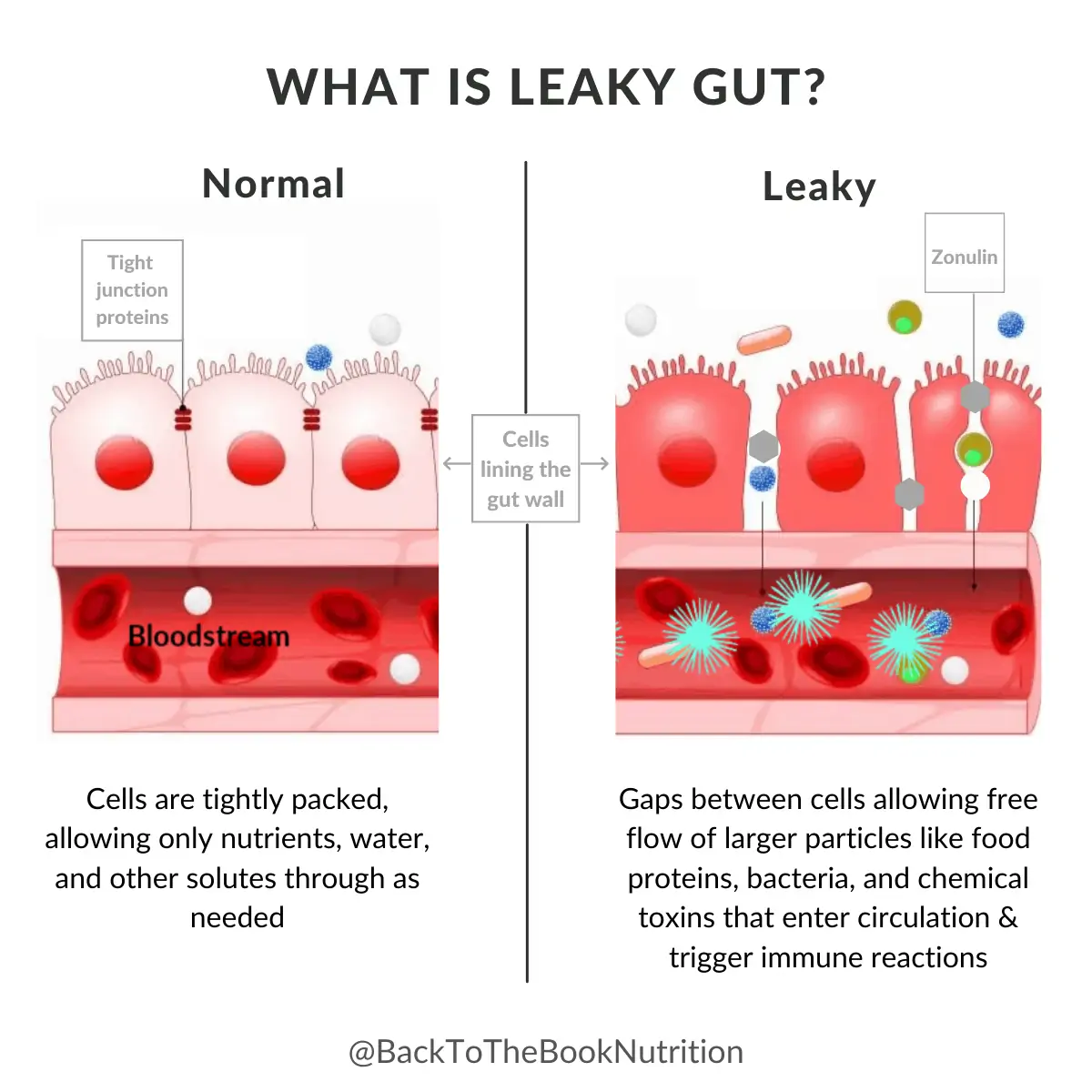
Our small intestines are lined with cells that create a barrier between the GI and the bloodstream. This barrier is held tightly together with proteins called tight junction proteins (1). Normally, these proteins act like “bouncers” at the door of a club, stationed at the “doorways” between cells of the intestinal wall. These bouncers select which items (water, nutrients, etc.) to allow to pass through and which ones (pathogens, poorly digested food proteins, etc.) to block from circulation.
Zonulin is a protein that can influence the tight junction proteins to be more or less selective. When they’re less selective, the openings in the gut wall widen and allow more undigested food, bacteria, and toxins to escape the gut, “leak” into the bloodstream, and travel throughout the body. This triggers an immune response that, if not corrected, can lead to other health conditions.
Although the start of leaky gut occurs in the intestines, increased permeability of other barriers in our body like the skin and brain go hand-in-hand with leaky gut. This is why the symptoms of leaky gut can appear in our hormones, skin, joints, mood, and behavior.
Leaky Gut Symptoms
The lining of your intestines is the first line of defense for toxins in your bloodstream. When things get into the blood, it triggers inflammation and immune responses that are seen all over the body. Because of that, leaky gut can present itself in many different ways (1,2,3). The most common include:
- Gas, bloating, or reflux
- Food sensitivities
- Skin rashes like acne, eczema, rosacea, hives, psoriasis, and perioral dermatitis
- Headaches or migraines
- Brain Fog
- Neurological issues like ADD, ADHD, tics, or depression
- Chronic Fatigue
- Muscle or joint pain
- Nutrient deficiencies
- Chemical sensitivity
- Allergies or frequent sinus infections
- No symptoms at all
Health conditions linked to Leaky Gut
GI DISORDERS (INCLUDING AUTOIMMUNE GI DISORDERS)
- Irritable Bowel Syndrome (IBS): All types of IBS are associated with leaky gut and dysbiosis, which is an imbalance of bacteria in the GI tract. Specifically, IBS-D shows a direct link to increased spacing between cells. (3)
- Inflammatory Bowel Disease (IBD): An umbrella term for Crohn’s and Ulcerative Colitis. In these autoimmune diseases, a defective GI lining creates inflammation in the digestive tract, which leads to further defects in the gut lining. (1,4)
- Celiac Disease: Celiac is an autoimmune condition where gluten consumption causes damage to the small intestinal lining, resulting in leaky gut, among other things. This can weaken the barriers of other body systems including the skin, explaining why skin rashes are common in Celiac patients. (3)
OTHER AUTOIMMUNE DISORDERS
Because leaky gut causes inflammation in the bloodstream, it is often a gateway to all forms of autoimmunity. Our body thinks something “foreign” is in our bloodstream that it must attack. For most autoimmune diseases, the cause-and-effect relationship between autoimmunity and leaky gut remain unclear. However, there is strong evidence of increased intestinal permeability occurring before, during, or after the onset of some disorders.
- Type 1 Diabetes: A leaky GI lining occurs before the onset of type 1 diabetes which allows bacteria leaking from the GI to go into the pancreas. This could be why GI pain and dysbiosis are often seen in patients before the onset of T1DM. (1,2,3).
- Hashimoto’s Thyroiditis: A gut-thyroid connection exists that helps the thyroid monitor and control our metabolism. When our thyroid function is weakened, this increases gut permeability and in turn, can further damage the thyroid. (5)
- Lupus: Lupus patients often see dysbiosis in the GI, which contributes to or possibly initiates the inflammation they experience in the whole body. (1,2,)
- Alopecia: Hair loss is often a sign of underlying inflammation. Although not always due to GI inflammation, leaky gut could be a contributing factor. (6)
- Rheumatoid Arthritis: An unhealthy microbiome and caused widespread inflammation such as arthritis. (7)
- Ankylosing Spondylitis: Dysbiosis in these patients is common, which increases zonulin that breaks down tight junctions, and further weakens the GI lining. (1,3)
- Multiple Sclerosis: Dysbiosis can contribute to the development of MS related nerve damage by weakening the GI barrier, and later the blood-brain barrier. (1,3)
- Fibromyalgia: Newer research links fibromyalgia to various GI imbalances (SIBO, IBS, etc.) as well as leaky gut. (34)
SKIN CONDITIONS
- Psoriasis: Psoriatic skin rashes are linked to dysbiosis and leaky gut. (8)
- Acne Vulgaris: When the intestinal microbiome is altered, it can relay inflammation to skin cells, increasing some cases of acne. (9)
- Dermatitis: Gut dysbiosis + a faulty skin barrier gives rise to dermatitis. (9)
- Eczema: Eczema is linked to dysbiosis and leaky gut. (35)
NEURO-INFLAMMATORY DISEASES
- Autism: Many people with ASD have high zonulin and respond well to leaky gut therapy if GI issues are already present. (3)
- Depression: Changes to the intestinal microbiome can impact communication to the brain (3)
- Schizophrenia: Specific bacterial imbalances, GI inflammation, and leaky gut are more common in schizophrenia. (33)
- Chronic Fatigue Syndrome: Although the cause of this disorder is unknown, dysbiosis and impaired GI function are present during the development of CFS. (3)
- Attention Deficit Hyperactivity Disorder (ADHD): Children with ADHD had higher zonulin, and the degree of zonulin elevation correlated with increased impairments in social function. (37)
- Alzheimer’s and Parkinson’s Diseases: Both of these conditions have been strongly linked to dysbiosis and markers of intestinal permeability. Early data suggest aggressive diet and lifestyle changes significantly improve cognitive abilities. (38)
CARDIOVASCULAR DISEASE
- Heart Disease: Several bacterial overgrowths and intestinal inflammation are both precursors to leaky gut that have been linked to heart disease – more study is needed to confirm the connection. (29)
- Pregnancy Induced Hypertension (PIH): A small study of pregnant women found those with PIH had significantly higher zonulin levels. (30)
METABOLIC DISORDERS
- Obesity: Obese individuals have higher zonulin than non obese. (32)
- Type 2 Diabetes: Patients with Type 2 Diabetes have higher zonulin levels than non diabetic individuals. (31)
- Polycystic Ovarian Syndrome (PCOS): This has historically been labeled as a hormone disorder, but more data is categorizing it primarily as a metabolic disorder, and linking it to inflammation, dysbiosis, and leaky gut. (32)
KIDNEY DISEASE
- Diabetic Kidney Disease: Higher zonulin levels were linked to lower kidney function and poorer outcomes in Type 2 diabetic patients compared to diabetics without kidney disease. (31)
ALLERGIES AND ASTHMA
- Allergies and Asthma: Chronic allergy and asthma are correlated to gut imbalances and increased intestinal permeability. (35)
NATURAL AGING
- Natural Aging Process: Zonulin is naturally higher in older adults compared to younger ones, even prompting a term called the “intestinal permeability theory of aging.” (37)
What Causes Leaky Gut?
Research is continually revealing more contributors to increased intestinal permeability, but here are some factors we currently know cause it, with gluten and dysbiosis being the strongest drivers according to current research:
Poor Diet
- High Refined Food Intake: Refined and processed foods are often high in inflammatory fats and low in fiber. Chronic high intake of these foods gives rise to harmful overgrowths and lower levels of healthy intestinal bacteria that make short-chain fatty acids (SCFA) to lower GI inflammation maintain gut integrity. (9,10)
- High Sugar Intake: Excess sugar is a source of inflammation and food for harmful gut bacteria. Chronic, high intake is directly related to dysbiosis in the gut. (11)
- Food sensitivities
- Gluten: Gluten increases zonulin, the protein that deteriorates the tight junctions. This can occur in Celiac patients as well as non-Celiacs. (12) Further, a gluten-free diet was found to restore the lining and regulate bowel movements in IBS patients (13)
- Dairy?: The whey protein in milk can cause damage to tight junctions and lead to increased permeability (12), but kefir has been shown in at least one study to lower zonulin. (36)
- Others: Sensitivities to any foods can raise GI inflammation and contribute to leaky gut.
- High alcohol intake: High intake of alcohol leads to a dysfunctional GI barrier and decreases the quality and quantity of healthy gut bacteria. (2,12)
- Nutrient deficiencies: Vitamin D, Zinc (12), Vitamin A (12,14), and protein are all essential in maintaining a healthy gut. Deficiencies in these nutrients can lead to a lack of tight junctions and a weakened immune system.
Bacterial Overgrowths
H.pylori, salmonella, SIBO, parasites, and other gut infections can inflame and wear down the GI lining. (1,2)
Not Enough “Good” Gut Bacteria
Beneficial bacterial strains in the GI tract such as Lactobacillus, Bifidobacter, Clostridia, and Akkermansia, are extremely helpful to maintaining a healthy GI lining. These bacteria help up by:
- Taking up real estate that would otherwise go to “bad” bacteria and yeasts, thereby preventing them from overgrowing
- Producing butyrate and other short-chain fatty acids (SCFAs) that help build a nice and thick intestinal lining
- Exerting immune activity to help fight off pathogens that would otherwise increase gut inflammation and wear down the lining.
Candida and other Yeast Overgrowths
Candida can actually cause a collapse of the brush border, which is the first layer of the GI lining. (1)
Glyphosate (Roundup)
This is the active ingredient in the herbicide, Roundup. This chemical causes dysbiosis and an increase in bacteria that break down tight junctions (15). It’s prevalent in non-organic foods and in unfiltered water as well. More research is needed to confirm whether other pesticides, herbicides, and fungicides have similar effects on the gut.
Stress
Chronic stress decreases digestive juices (stomach acid, digestive enzymes, etc.), making it harder to break down foods, increasing the risk for food sensitivities as well as bacterial or yeast overgrowths. These as well as the direct impact of stress on the gut lining, can promote leaky gut. There are two types of stress:
- Mental and emotional stress like anxiety or chronic mental stress. This slows down the immune system by making it harder for your body to heal (1)
- Physical or oxidative stress like inflammation, excess body weight, poor blood sugar control, poor sleep, and over-exercising. (1)
Poor Sleep
Sleep disruption is linked to lower melatonin and dysbiosis, which both promote leaky gut. Lack of sleep is also associated with a bacteria called lipopolysaccharides that cause brain fog and fatigue. (10,16)
Medications
- Antibiotic Use: antibiotics kill off both healthy and unhealthy bacteria in the gut in an effort to kill the source of infection. This massive cleanout of bacteria creates an imbalance or dysbiosis. Long-term antibiotic use will kill off too much of the healthy bacteria.
- PPIs like Prilosec, Prevacid, Nexium, Prilosec, etc.: chronic use can reduce acid levels in the stomach too much, making it more difficult for the GI to fully break down food.
- Antacids such as Pepcid or Tums: along with PPIs, also can reduce overall acid levels in the stomach
- Birth control long term: years of usage creates an environment in the gut favorable for fungi growth that damage the GI lining (1)
- Pain medications, including NSAIDs (ibuprofen, Advil, Motrin, etc.), Tylenol, aspirin, and opioids (morphine, Hydrocodone, etc.). Chronic use can impair the border of our intestines, which allows for undigested food to enter the bloodstream
- Chemotherapy: breaks down gut lining while trying to kill off cancer cells (1)
Mold and Mycotoxins
Prolonged exposure to molds or mycotoxins (the harmful chemicals molds emit) can change the makeup of our microbiome and even lead to microbial infections in the GI tract. (17,18).
Tests for Leaky Gut
Unfortunately, there is no perfect test to diagnose leaky gut, and it cannot physically be seen in endoscopies or colonoscopies. Below are the most accurate testing options we have currently:
GI MAP + ZONULIN: An easy, at-home stool sample collection by Diagnostic Solutions Lab (zonulin section from one of my clients pictured above)
- Tests the entire microbiome profile for 85+ different markers including H.Pylori, bacterial overgrowths, yeasts, parasites, and other issues that often require a more targeted protocol in addition to diet and lifestyle change
- Also identifies high zonulin levels, the protein we talked about earlier that promotes larger gaps in the GI lining.
GUT ZOOMER: Finger prick blood test by Vibrant Wellness Lab
- Tests for zonulin antibodies, beta-defensin 2, celiac disease, and wheat sensitivity
ZONULIN ONLY TEST (stool or blood): Some practitioners and physicians offer this single marker test to gauge intestinal permeability. Your practitioner will choose whether to use a stool sample or a blood draw is more effective.
LACTOSE MANNITOL TEST: This is the gold standard among conventional medical practitioners. You drink a sugar solution of lactose and mannitol, then collect urine a few hours later to reveal levels of intestinal permeability. (19)
Not ready to test, but want to know if you have leaky gut? Take this quiz!
How to Fix Leaky Gut
Repairing a leaky gut lining is all about removing things that are hurting it and adding things to help it.
1. Eat a gut healthy diet
Eat to maximize nutrients that promote a healthy GI lining as well as to minimize dietary triggers of leaky gut, including these:
INCLUDE THESE GUT HEALTHY NUTRIENTS:
- Vitamin D: fish, chicken, eggs, mushrooms, fortified milk
- Vitamin A: carrots, tuna, sweet potato, red bell peppers, meat, cheese, eggs
- Zinc: oysters, beef, lentils, hemp seeds, oatmeal, yogurt, tofu
- Omega-3 Fatty Acids: fatty fish like salmon, nuts, seeds, avocado
- Protein: meats, poultry, fish, eggs, beans, peas, and legumes
EAT ENOUGH PREBIOTIC FIBER:
Think of prebiotics as the necessary food for probiotic organisms to eat so they can help build up our GI lining and promote overall digestive health. (12) Prebiotics are a type of soluble fiber and are naturally found most plant foods. But these foods are especially high:
- onions, leeks, and shallots
- asparagus
- beans, peas, and lentils
- oats/oatmeal
- apples, bananas, berries
- cashews and pistachios
INCLUDE FERMENTED FOODS
Fermented foods are rich in probiotics which help control the growth of bad bacteria, reduce inflammation, and help moderate immune activity. (1)
- Yogurt and kefir (ideally plain or lower sugar varieties; includes non-dairy versions)
- Kimchi
- Natto
- Traditionally prepared sauerkraut, pickles, carrots, and other fermented veggies
- Kombucha (if buying, choose those with lower sugar content)
EAT POLYPHENOL RICH FOODS
Polyphenols help feed good bacteria that produce short chain fatty acids (SCFA’s) to maintain gut integrity. They are also antioxidants that help repair oxidative damage in the body. (12)
- Berries
- Raw cacao (powder, nibs, etc.) and dark chocolate
- Plums
- Cherries
- Apples
- Pomegranate
- Beans (especially black beans)
- Black and green tea (regular and decaf)
- Coffee (regular and decaf)
- Extra virgin olive oil
- Ground cloves
EAT GELATIN AND DRINK BONE BROTH
Bone broth and gelatin have traditionally been used to soothe digestion. These are notably high in is high in anti-inflammatory amino acids like proline, arginine, glycine, and glutamic acid (glutamine) that support gut integrity. However, bone broth also contains histamines. If you are sensitive to histamine, use gelatin, which is histamine free, instead.
EAT BITTER FOODS
Bitter foods can help you make more stomach acid and digestive juices to break down your foods better, limiting the risk for food sensitivities and bacterial overgrowths, both of which promote leaky gut. These can be in whole food, dried spice, or tea form.
- Artichoke
- Dandelion, mustard greens, beet greens
- Arugula
- Endive
- Fennel
- Ginger
- Peppermint
- Chamomile
- Cinnamon
EAT ORGANIC
Organic produce has much lower amounts of glyphosate and other pesticides and herbicides that promote leaky gut. (15)
CONSIDER GOING GLUTEN FREE
Gluten has been shown to negatively impact the GI lining even for those without Celiac Disease. A trial period of a gluten-free diet may help resolve leaky gut and could help you decipher if gluten is causing some of your main symptoms.
AVOID KNOWN FOOD SENSITIVITIES AND INTOLERANCES
GI-triggering foods are different for everyone. Try keeping a food journal documenting your diet and symptoms for at least one week to help identify food sensitivities. Common foods that cause GI discomfort include dairy, wheat, gluten, onions, garlic, and cruciferous vegetables. (2,12) Working on your gut issues could potentially help you tolerate these foods again.
LIMIT ALCOHOL AND REFINED SUGAR INTAKE
Both of these which can worsen GI symptoms and cause disruption to the GI lining, especially when consumed in larger amounts. Limit yourself to no more than one drink per day for women or two drinks per day for men, and less than that may be even better.
2. Test for and fix gut infections
Work with Dena to order a GI MAP + Zonulin comprehensive stool test to identify gut infections like SIBO (small intestine bacterial overgrowth), H.pylori, Candida, etc. and to test markers of leaky gut and healthy digestion. Objective test data helps us create a targeted plan for your specific imbalances to get you the best possible results.
3. Eat slowly and without distractions
Eating on the go or in a rushed state decreases digestive juices, making bacterial/yeast overgrowths, food sensitivities, and leaky gut more likely. Download my free Meal Time Checklist to help!
4. Reduce and Manage Stress
As mentioned earlier, stress increases inflammation, significantly reduces digestive juices, and increases intestinal permeability. Refer to the Ultimate Stress Management Guide to help identify personal stressors and create a stress management plan.
5. Get Great Sleep
Aim for at least 7 hours of good quality sleep each night. This minimizes the risk for inflammation, cortisol imbalances, and dysbiosis that can drive leaky gut. Can’t sleep? These 20+ natural sleep tips and supplements to help!
6. Exercise Regularly, but don’t overdo it
Consistent exercise over weeks or months reduces markers of intestinal permeability. (20) But, as mentioned above, workouts that are too intense can add stress to the body – especially if you don’t take enough rest days. (21) If workouts leave you feeling wiped out for hours afterward, adjust your routine to include movement that builds strength, increases energy, and allows for a full recovery.
7. Evaluate your medications
Ask your doctor about alternatives or dose adjustments of medications that weaken the GI lining mentioned above (aspirin, ibuprofen, PPIs, birth control, pain medications, etc. ). If adjusting your meds isn’t possible, be extra attentive to the other tips on this list to minimize your risk of leaky gut.
8. Remove Mold and Mycotoxins
If your home, office, car, or other area where you spend a lot of time has a history of water leaks or mold, these may be contributing to leaky gut. Even previous exposures can still be affecting you. Unfortunately, it’s nearly impossible to fully heal if you’re still regularly exposed to mold/mycotoxins. To fully recover, you must both repair mycotoxin damage in your body and properly remediate or remove yourself from the moldy environment.
9. Consider gut supportive supplements
To be clear, no one needs all of the supplements listed here to fix leaky gut. But a few, in combination with other products targeting specific types of overgrowths and support digestive juices like stomach acid and enzymes, can be very helpful. Always consult with your own healthcare provider before starting new supplements.
- Glutamine: food for our intestinal cells to “heal and seal” while also reducing intestinal inflammation (22)
- Vitamin A: Multiple human studies have linked low vitamin A to alterations in gut bacteria and intestinal lining. (14).
- Vitamin D: protects intestinal permeability and is especially helpful for Crohn’s patients (2,23)
- Fish oil: a great source of omega-3, which acts to lower GI inflammation.
- Quercetin: one type of polyphenol, which help maintain gut integrity
- Reds powders: beet powder or combination powders that include a variety of deep red fruits and veggies are rich in polyphenols that feed the good bacteria to increase butyrate and other SCFAs to maintain a healthy intestinal lining.
- Collagen powder: collagen production is needed for the maintenance and healing of the GI lining. It is high in amino acids like glycine and glutamate that keeps the lining healthy (24)
- Zinc carnosine: Especially if you are deficient in zinc and not eating enough zinc-rich foods, it can be helpful for healing the mucosal lining
- N-acetyl glucosamine: helps to restore the integrity of GI lining and mucus production (25)
- Prebiotics: inulin, guar gum (PHGG), and acacia gum (1)
- Probiotics: These help combat yeast and bacterial overgrowth, calm inflammation, and support gut immune function. Learn how to pick the right probiotic here.
- Colostrum or Immunoglobulins: these have been shown to reverse some of the GI damage from repeated NSAID medication use (26) as well as decrease intestinal permeability (27)
- Butyrate: If you have low levels of healthy bacteria that produce butyrate, taking a butyrate supplement may speed up gut-healing while you work to build up your healthy bacteria. Few studies have been done, but it’s a low-risk consideration.
- Other Supplements that help calm gut inflammation and soothe the GI lining (28):
- Slippery elm
- Marshmallow Root
- Licorice root
- Aloe
- GI Resolve, and DGL Plus pictured above combine a few of these items into a single product.
Buy Leaky Gut Supplements Here!
How long does it take to fix Leaky Gut?
Long story short – it depends. To fully resolve leaky gut, the root cause needs to be addressed. Depending on the underlying conditions, usually, a minimum of 3 months of diet modifications, supplements, and lifestyle changes are necessary, but it can take much longer for more complex cases.
Working one-on-one with a practitioner who specializes in gut health can give you a personalized plan with the best results.
Schedule your free Discovery Call & let’s fix your gut!
About the Co-Author:
Lauren McNamara is currently a dietetic intern at the University of Houston. She graduated from the University of Texas at Austin with a degree in nutrition and child-family development. Lauren has a strong interest in maternal and infant nutrition, as well as helping families develop healthy habits. In her free time, she enjoys cooking, baking, and running.
Disclaimer: Information on this site is intended only for informational purposes and is not a substitute for medical advice. Always consult with a trusted healthcare provider before implementing significant dietary change. Read additional disclaimer info here.
References:
Read More











I would imagine that with most western diets, especially in an American diet, we are more prone to having a leaky gut which is unfortunate. Thank you for the information.
You’re right – Nkem. Thankfully there’s a lot we can do to repair it!
Hhhmmmm….to be honest, I report over 9 of the symptoms mentioned here in this blog post for leaky gut. A doctor should check me out as soonest as possible!
Wow! I learned something new about leaky gut. It’s so important to know more about it. Thanks for the additional info! Very informative!
You’re welcome – thanks for reading and for your comment!
Great post. There is so much good info here.
A lot of information about the leaky gut. This would help a lot of people who suffer from this and you went through it smoothly. Thank you for sharing!
Fransic – https://www.querianson.com/
I have diabetes and this is more of an awareness to me. I do have problems too with my gut due to my diabetes.. Although i do not know if i can link it to a leaky gut but the possibility is high. I was advised to have a balance diet and make sure my sugar level os regularly checked
So good that you’re aware of your diet and gut health, Milton – both very important for diabetes!
Definitely a lot you can do! 🙂
It’s super hard when one of the symptoms could be ‘no’ symptoms. It’s frustrating to the doctor(s) and the patient, and such a relief when a true diagnosis is made.
You’re so right, Rosey. I’d say most people do have symptoms of Leaky Gut, but it’s good not to rule it out even if symptoms aren’t present.
Very interesting. I’ve heard of this before but never knew this much detail.
An unhealthy gut indeed can cause many physical ailments. I’ve learned a lot from your post and as I read it, I can’t help but think that many of our diseases are probably due to a leaky gut.
Very true, Ivan.